In total, 93 participants attended an interview or focus group across regional (n = 6) and remote (n = 4) healthcare systems (Table 1).
Perceptions of rural digital health capability
The perceptions of digital health capability dimensions in rural healthcare systems are described below. Three new sub-dimensions were identified; resources (governance and management dimension); fit-for-purpose (IT capability dimension); and attitudes (people, skills and behaviour dimension). Appendix 3 provides additional evidence of the capability subdimensions.
Consumer-centred care, in terms of supporting consumers to manage their own health through technology-enhanced care and improved consumer health literacy, was valued by participants: “Communication with patients, so the ability to send text messages or have an app that allows them to track their own health, in terms of appointments, results, medications …would be …great.” (G6). Limited resourcing, time availability and dispersed location of consumers were described as barriers to the access and use of technological infrastructure needed to enable consumer-centred care.
Governance and management were considered vital as rural sites transitioned from paper to digital. Adequate resourcing and support for staff through this transition was important: “In …the last five years, we’ve introduced them (staff) to [the electronic medical record] and that has been a huge challenge with a lot of change initiatives and management to …bring them along on the journey.” (E2). Participants identified that governance and management efforts should be targeted at providing effective data governance, protocols for sharing data with external providers, and reducing unsafe workarounds.
In the IT capability dimension, digital infrastructure was limited by internet connectivity: “The other barrier …is our connectivity within our sites, with being rural and remote. We don’t always have the greatest internet. …Our bandwidth and our speed [is poor]” (F8). During transition phases, participants reported the ‘hybrid’ paper-digital model resulted in duplicated information and poor data accuracy. The use of dashboards was valuable for visualising data.
In the people, skills and behaviour dimension, the digital literacy of the healthcare workforce mediates their acceptance of digital health: “The hardest thing was they’re extremely experienced and knowledgeable clinicians, and they’ve had to now go into something where they feel inadequate and feel that they can’t do their job” (E1). Participants indicated that the continued use of telehealth and investment in education to enhance individual competence and clinician confidence in digital technologies can minimise unnecessary workarounds and contribute to providing equitable care to rural populations.
Interoperable systems were perceived to facilitate efficient and accurate exchange of clinical information. Continuity of care is difficult between primary care providers, state-funded health services, and external providers in rural settings: “I can see a benefit in patient care delivery for when the entire health service is on the same system, because it will help with the transfer of the patient care through the different journeys” (B4). Participants emphasised that poor information visibility with external providers limited external interoperability, and the numerous systems utilised within a healthcare system limited internal interoperability.
The strategic focus of rural healthcare systems is interoperability, digital competency and investment in education and training. Strategic adaptability and alignment to organisational strategies is reported as challenging in rural contexts as digital health solutions were originally tailored for other healthcare systems in Queensland: “The state-wide solutions don’t really cater for the [rural health], because of how isolated and remote it is” (J10).
Rural healthcare providers use data analytics for healthcare performance tracking. Accurate data input by clinicians was critical for data analytics: “[The digital system] is our source of truth and it needs to be correct and up to date because that’s where all of our information from a funding perspective comes from” (B3). The continued use of paper is required for manual auditing. Participants saw value in extending data analytics to provide insight into trends and identify clinical risks, particularly for chronic disease management.
Relationships among digital health capability dimensions and outcomes
All four healthcare outcomes (population health, patient experience, provider experience, and healthcare costs) were described to be influenced by the digital health capability dimensions (Fig. 3; Table 2, Appendix 4). Strategy did not directly impact any outcome.
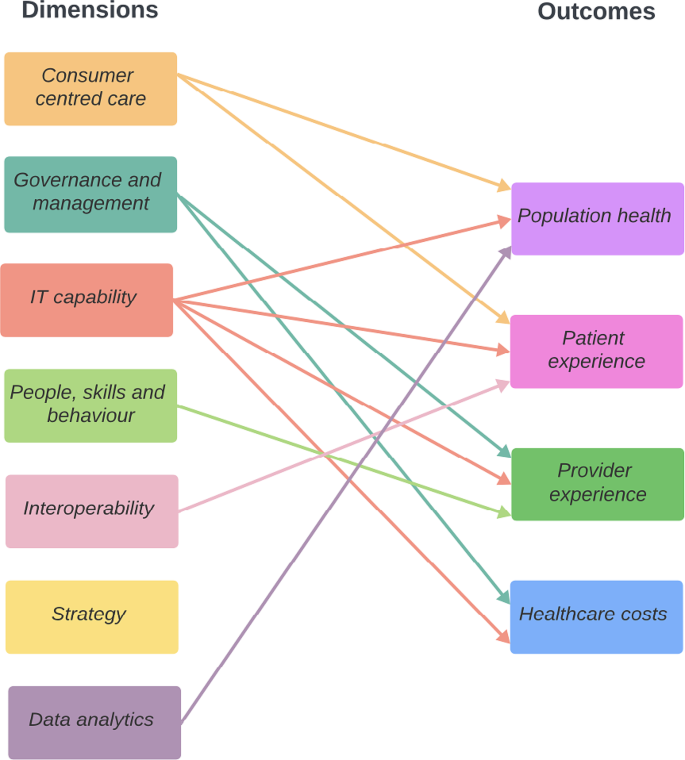
Dimensions of digital health capability and their relationships to the healthcare outcomes
Relationships among the digital health capability dimensions
Interrelationships were present among all digital health capability dimensions (Fig. 4, Appendix 5).
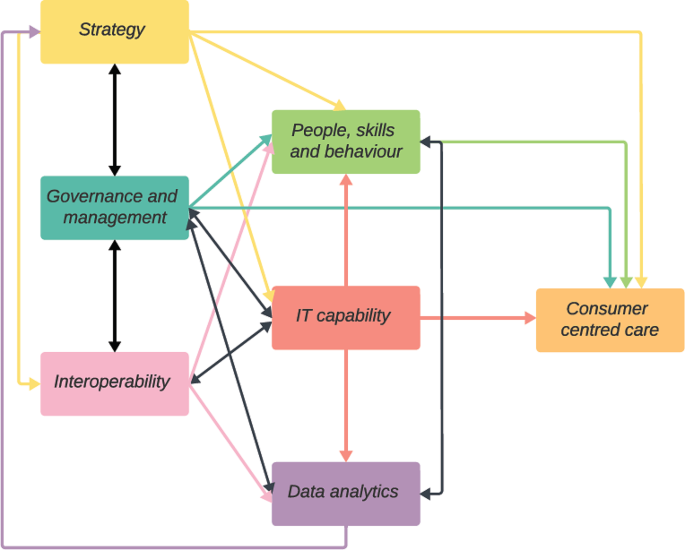
Interrelationships among the digital health capability dimensions
Participants described the strategy dimension influenced the governance and management, people skills and behaviour, IT capability, interoperability and consumer-centred care dimensions. To incorporate digital transformation in the strategy and facilitate “care closer to the home” (J4), monetary and human resources are required. Enacting the digital strategy requires balancing priorities to develop the digital capability of the health system and “invest in the education and training of staff” (F7) to improve people, skills, and behaviour. Investment in technology infrastructure is required: “to invest in any further digital transformation, [it] must come with updated hardware infrastructure” (F6). Interoperability was core to the strategy, with the vision to “have one system, …so …all of our users …are only seeing one system, and if that’s not possible, then get interoperability front and centre on everyone’s roadmap” (G2).
Participants reported the challenge of governance and management and described its influence on all dimensions. Resource constraints and a lack of digital health governance within individual healthcare systems have hampered the digital health strategy from being realised. Implementation of technologies (e.g., telehealth) and structures (“consumer and community engagement team” (I6)) to facilitate consumer-centred care have been introduced in rural settings. Due to the segmentation of healthcare systems and primary and secondary care, participants expressed the importance of interoperability standards: “blanket rules that all digital platforms …talk(ed) to each other” (B6). In some instances, efforts to improve interoperability have been introduced by management, ensuring that the same system is used across sites: “Patient flow manager for us is our communication tool and we made sure that every site has [it]” (D12). Despite “government documents that dictate how it should be used, …they’re not well enforced” (F8) and individual variations exist in technology use. Establishing a “culture …[that] supports very open and transparent reporting of incidents” (A7) and structures such as a “business analysis and decision support team …[and] a nurse informatics [area]” (B10) facilitated data analytics.
IT capability influenced the governance and management, data analytics, consumer-centred care, people, skills, and behaviour, and interoperability dimensions. Governance and management were facilitated by providing “a full audit system …we can audit, we can review, we can look at gaps” (F8). IT also enabled analytics: “we use [software] to collate and to present data back to clinical teams, …for decision making, …to understand trends, …[and] for reporting …to the board and executive” (I6). Leveraging the capability of web-based portals, community healthcare directories, and telehealth have “enabled deeper engagement with the community” (F9) facilitating consumer-centred care. In some instances, IT improved interoperability: “we can see every admission to a public hospital in Queensland, and clinical notes, and discharge summaries” (B2). However, other IT did not meet interoperability standards and, the inclusion of additional IT was sometimes met with fear and frustration.
Interoperability influenced the governance and management, data analytics, people skills and behaviour, and IT capability dimensions. Participants expressed frustration with the limited interoperability: “instead of having one single channel which is commonly shared by everybody, we now have five different variants at both ends” (A3). Suboptimal interoperability impedes IT capability and data analytics: “if everything is linked to all databases, …you [would] have these wonderful capabilities to put your parameters in and run a report” (D9). Participants noted that a lack of interoperability between state-wide systems is “fraught with risk” (C9) that need to be managed.
Participants described how data analytics influenced the strategy, governance and management, and people, skills, and behaviour dimensions. Reporting and visualisation of data facilitated “operational and strategic planning” (J8). Data analytics can be used to actively monitor whether national standards are met: “We have a national standard called Emergency Length of Stay – …making sure patients leave within four hours. …I use the [digital] system …to keep tracking ‘where are we at? What’s our timing, what are we doing’” (E1). However, individuals had a “sense that the data will be used against people” (D6) and expressed concerns “over being a micro-manager” (D4).
The consumer-centred care dimension did not influence any digital health capability dimensions.
People skills and behaviour appeared to influence the data analytics and consumer-centred care dimensions. Healthcare professionals perform workarounds to overcome system limitations, often resulting in poor data quality hampering data analytics: “garbage in, garbage out. …Because people didn’t enter information correctly, it … threw out the whole dataset.” (E9). Digital health literacy of healthcare professionals and consumers influenced the delivery of consumer-centred care: “To access healthcare moving forward you will have to have a level of digital acuity and we need to be responsible for building competency and checking for competency. …It’s not just for the patients, …it’s a skill that we need to embed with our staff.” [B7].
link

